The Great Libido Lie: Women Don’t Lose Desire — They Lose Safety, Energy, and Time.

By Berta Kaguako, Mental Health and Substance Misuse Consultant
Introduction
With women’s health awareness in mind, it’s important that we start honouring shared female experiences, as these aren’t just shared by some, but by the majority of women.
As a 38-year-old woman, I grew up being told to shoulder many things and to chip away at myself in order to conform to societal and cultural pressures! Over time, I stepped into the role that was expected of me, carrying responsibilities that followed me into daily life.
Sadly, regardless of your race, age, or cultural background, the one thing we can all unite on is that we all had this experience, each and every one of us. For many women, professional obligations must be met to the same standard as anyone else’s, often under greater scrutiny and with less flexibility. At the same time, they often carry the greater share of responsibilities at home, from raising children and managing households to supporting the emotional stability of the family. In many cases, this extends to caring for aging parents while continuing to manage finances, logistics, and the unseen labour that keeps daily life functioning. This accumulation of responsibilities carries a significant emotional and practical weight. While these roles are often accepted out of commitment to family and stability, they nonetheless reflect expectations that place a disproportionate burden on women. We lose ourselves to the desires of others, and we don’t notice that our hearts have closed up over the years, and that is the start of the tipping point.
As somewhere in the middle of holding everything together, a quiet shift begins inside the Body.
Desire fades
Intimacy becomes a chore
Passion starts to feel distant and/or unwelcome
Stress starts building up
Affection is withdrawn as you allow yourself to enter a more fight/flight state
For many women, this change arrives just as their bodies begin transitioning toward perimenopause, a hormonal stage that can start years before menopause itself. Add in modern stress, mental health challenges, chronic illness, and the emotional demands of adulthood, and it becomes clear why so many women find themselves asking a difficult question: Where did my libido go?

By the time many women reach their late thirties, the mental load alone can begin to feel overwhelming, just as the body is transitioning into perimenopause.
Perimenopause can start as early as the mid-thirties and is associated with fluctuating levels of estrogen, progesterone, and testosterone: hormones that influence sexual desire, mood stability, energy levels, sleep quality, vaginal lubrication, and emotional sensitivity.
Many women report feeling as though they are suddenly living in a different body: one that feels more tired, less responsive, and less interested in sex. Yet this experience is rarely discussed openly. Instead, women often internalise the change as though something is wrong with them.
But libido is not simply about attraction or romance. It is deeply connected to mental health, physical wellbeing, hormonal balance, and nervous system regulation.
The Hidden Connection Between Mental Health and Libido for Women
Reduced libido is often an early sign of declining mental wellbeing. Conditions such as chronic stress, anxiety, depression, burnout, and emotional trauma can suppress sexual desire by activating the sympathetic nervous system, the body’s fight-or-flight response, which prioritises survival over pleasure. Elevated stress hormones like cortisol and adrenaline make it biologically harder to access relaxation, bonding, and intimacy, making sexual desire biologically harder to experience.
Medications commonly prescribed for mental health, including SSRIs and other antidepressants, can also reduce libido, sometimes compounding emotional frustration. Together, these factors can create a reinforcing cycle in which stress, emotional strain, and reduced sexual desire feed into one another.
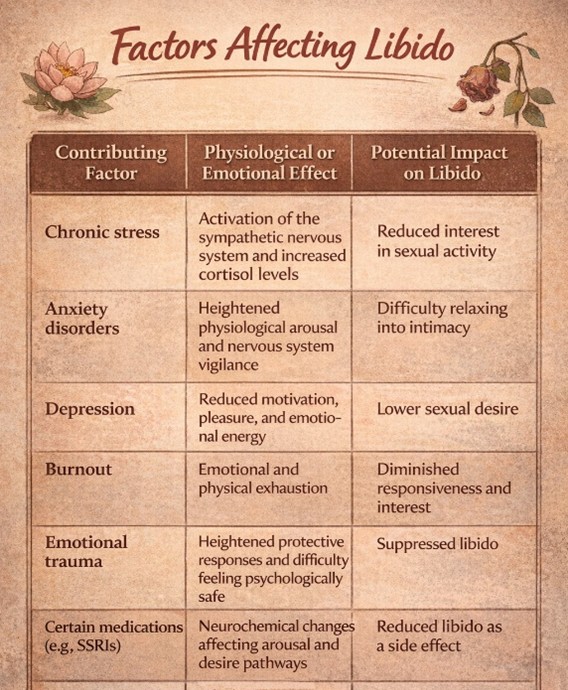
This interaction highlights how closely sexual desire is tied to overall wellbeing. But mental health is only one piece of the picture.
Chronic Illness and Female Intimacy
For women living with chronic illness, sexual wellbeing can be particularly affected. Conditions such as chronic pain, autoimmune or neurological disorders, hormonal imbalances, and mental health challenges can influence libido through multiple overlapping pathways, impacting both body and mind. Physical symptoms like pain, fatigue, medication side effects, and reduced mobility can make intimacy feel difficult or less appealing. Emotional responses to illness may also create distance from one’s body, leading to feelings of disconnection, frustration, or even betrayal when the body no longer responds as it once did.
Despite these barriers, many women still desire intimacy, emotional closeness, and the sense of feeling sensual, alive, and feminine. Managing symptoms can help improve both desire and comfort during intimacy.
Common Chronic Conditions That May Affect Libido
Chronic pain disorders
Autoimmune diseases
Neurological conditions
Hormonal disorders
Mental health conditions
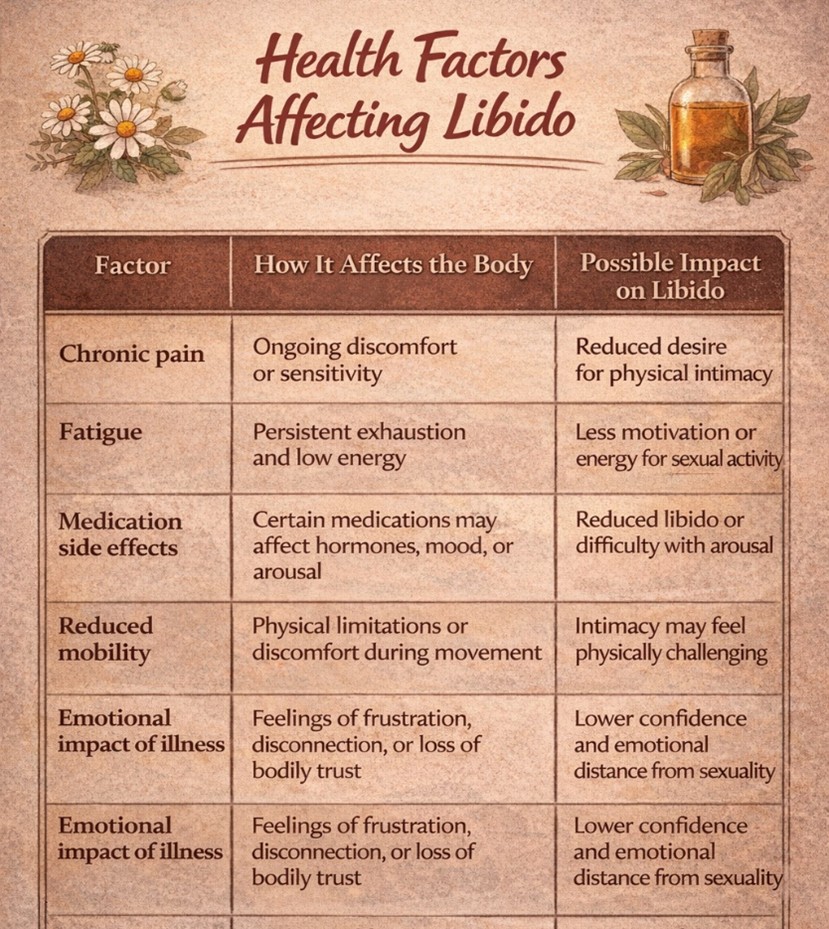
Other Factors That Can Decrease Libido in Women
Female libido is influenced by a complex interplay of biological, psychological, and lifestyle factors. Hormonal changes during perimenopause and menopause can alter oestrogen and testosterone levels, directly affecting sexual desire. Physical factors such as chronic fatigue, poor sleep, and chronic illness can further reduce energy, comfort, and interest in intimacy. Emotional and psychological influences are equally important. Body image concerns, emotional disconnection, and persistent stress can all suppress desire, especially when the mind is overloaded. Over time, some women may emotionally shut down—not intentionally, but as a protective response when the nervous system remains in prolonged survival mode.
Common contributing factors include:
Hormonal changes
Chronic fatigue
Poor sleep
Chronic illness or pain
Body image concerns
Emotional disconnection
Stress overload
These overlapping factors can gradually create distance between women and their sense of sensuality or desire.. However, this does not mean the longing for intimacy disappears. Many women still seek closeness, connection, and the ability to feel present and comfortable within their bodies. This is where an emerging area of research and increasing patient experience is beginning to draw attention: Cannabis.
Cannabis, the Endocannabinoid System & Women’s Libido
Cannabis interacts with the body through a biological network known as the Endocannabinoid System (ECS), which plays a key regulatory role across multiple physiological processes that influence overall wellbeing and sexual health. The ECS helps maintain balance by regulating mood, stress, pain, sleep, inflammation, hormones, and sexual function, all of which are closely linked to libido. By supporting emotional stability and reducing stress, it helps create the conditions where desire can emerge. The ECS also influences pain perception, making physical intimacy more comfortable, and regulates sleep cycles, which, in turn, support hormonal balance and energy. Its role in controlling inflammation can improve overall physical comfort, while interactions with endocrine signalling help maintain hormonal stability, a key factor in sexual desire. The ECS is also directly involved in sexual function, influencing arousal, pleasure, and sensory experience. Two of the most well-known cannabinoids, CBD (cannabidiol) and THC (tetrahydrocannabinol), interact with the body in different ways and may influence sexual wellbeing through distinct mechanisms.
Female Sexual Wellbeing: CBD vs THC
CBD is non-intoxicating and supports relaxation, emotional openness, and presence, while THC is intoxicating and can heighten sensations, boost pleasure, and make intimacy feel playful and adventurous. Understanding how each works can help women explore which cannabinoid, or combination, enhances their sexual experiences.
CBD and Emotional Intimacy
CBD is all about calm, connection, and presence. By reducing anxiety, relieving stress, and regulating the nervous system, it allows women to feel emotionally grounded and open during intimacy. Sexual desire in women is often responsive rather than spontaneous, meaning it arises when emotional safety, connection, and relaxation are present. CBD creates the ideal state for that to happen.
Heightened sensual awareness, noticing every brush, kiss, or caress.
During sex, this can translate into deep emotional connection, slow and deliberate pleasure, and feeling fully in the moment. Some women describe it as feeling more loving, attentive, and connected, like every touch is amplified by emotional safety and presence. It’s not about wild spontaneity: it’s about rich, responsive desire and intimacy that lingers long after the moment.
THC and Heightened Sensory Experience
THC, by contrast, is about play, sensation, and bold exploration. In low doses, it can amplify every nerve ending, increase tactile sensitivity, and make physical pleasure feel intense. Dopamine release and relaxation work together to make the body more responsive and adventurous.
Women using low-dose THC report:
Heightened physical sensations—touch feels electric
Enhanced arousal and responsiveness
Greater playfulness and spontaneity during intimacy
Feeling more adventurous and “rowdy”, bringing energy and exploration into the bedroom
Reduction in pain and discomfort, making intimacy more enjoyable
During intimacy, THC can shift the experience from routine to something more sensory, spontaneous, and physically engaging.
Dosage matters: higher doses can cause anxiety or sedation, so mindful, low-dose use is key to maintaining pleasurable, connected intimacy.
Bottom Line
CBD and THC each bring something unique to the bedroom. CBD anchors you in your body, enhances emotional closeness, and allows responsive desire to surface, while THC turns up the volume on sensation, heightens arousal, and invites playful exploration. For women with chronic illness, either or both can help bridge the gap between mind, body, and emotional connection, making intimacy feel possible, pleasurable, and deeply satisfying again.
A Gentle Reminder for Women Everywhere
If life has made your heart feel closed, if stress has made your body feel distant, or if intimacy feels like something from another chapter of your life, know this: you are not broken, and you are not alone. What you are experiencing is real, valid, and deeply human. Often, it simply means it is time to return to yourself, to reconnect with your body, your mind, and your heart.
You still have it—your desire, your sensuality, your curiosity—they’re just waiting for the right conditions to be welcomed back. Start with small, gentle steps: adjust your lifestyle, care for your mind, move your body, prioritise emotional connection, and regulate stress. Supplements like CBD, available over the counter in many places, can help calm the nervous system, reduce anxiety, and support emotional presence, creating space for intimacy. Beyond that, adaptogens, herbal medicines, mindful movement, and simple self-care routines can all help you feel grounded and attuned to your own body again.
It’s normal to feel vulnerable or hesitant. Sexual wellbeing is personal and precious, and for too long, women’s experiences have been overlooked. But there is hope—you can reconnect, rediscover pleasure, and rebuild intimacy on your own terms. You are seen. You are heard. You are deserving of love, connection, and care. Your sensuality hasn’t gone anywhere; you just need to find it again, gently, step by step.
Call to Action:
Learn about your body, mind, and the factors influencing sexual wellbeing.
Explore holistic approaches, including lifestyle, emotional, and plant-based strategies.
Advocate for more research into women’s sexual health.
Special Note for Women with Chronic Illness
For women managing chronic pain, fatigue, autoimmune conditions, or other long-term health challenges, both cannabinoids can be particularly beneficial. CBD can reduce anxiety and stress, helping women feel emotionally present and comfortable with intimacy. THC can enhance physical pleasure, reduce discomfort, and heighten sensory responsiveness, making sexual experiences more enjoyable despite physical limitations. Together, they can help overcome some of the barriers chronic illness creates between mind, body, and emotional connection.
About Berta Kaguako:
Berta Kaguako is a Mental Health and Substance Misuse Consultant with an Undergraduate in Psychotherapy and a Master's in Psychoanalysis. Berta’s background is in Mental Health, Substance Misuse and Children & Families: in both a therapeutic and senior management capacity, having won 3x Blooming Strong Awards (Recognition from UN for contribution to violence against Women). Berta is also the Co-Founder and Managing Director for EthVida, and independently runs the wellbeing service / educational platform.
Click the Learn More Button